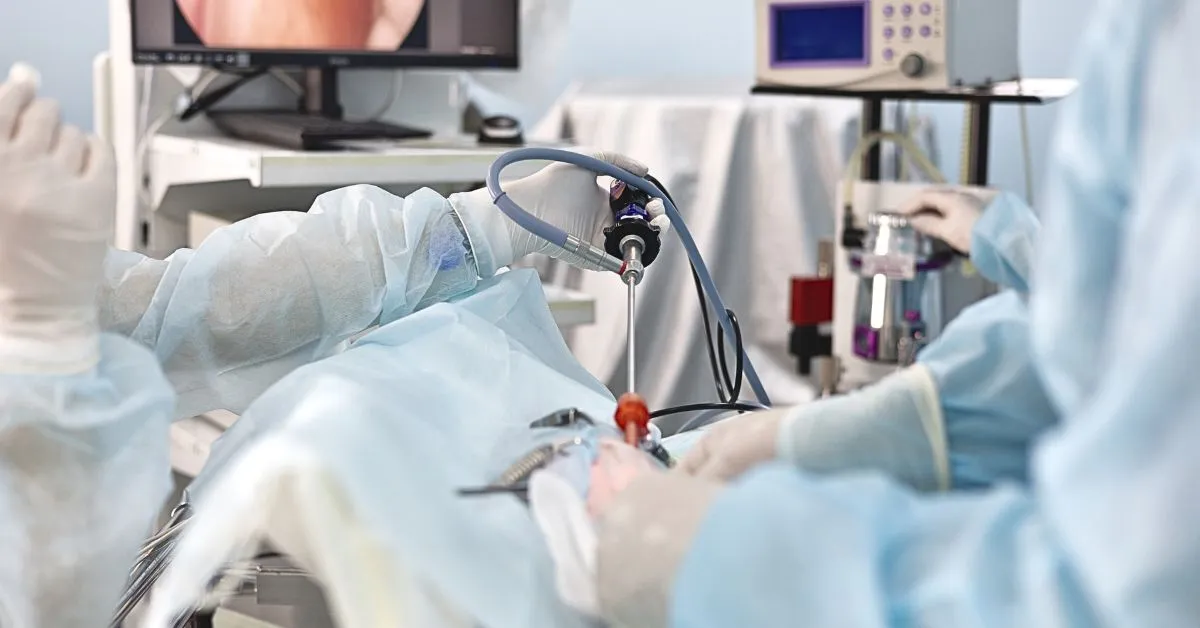
Meniscus injuries are common, especially among athletes and active individuals. These injuries can lead to significant pain, reduced mobility, and long-term joint damage if untreated. The meniscus plays a crucial role in shock absorption, load distribution, and joint stability within the knee. Repairing a torn meniscus is often preferred over removal to preserve knee function and prevent osteoarthritis. Platelet-Rich Plasma (PRP) therapy has emerged as a promising adjunct treatment to enhance meniscus repair outcomes. This article explains the role of PRP in meniscus repair surgery, presenting evidence, benefits, and limitations.
What Is PRP Meniscus Repair Surgery?
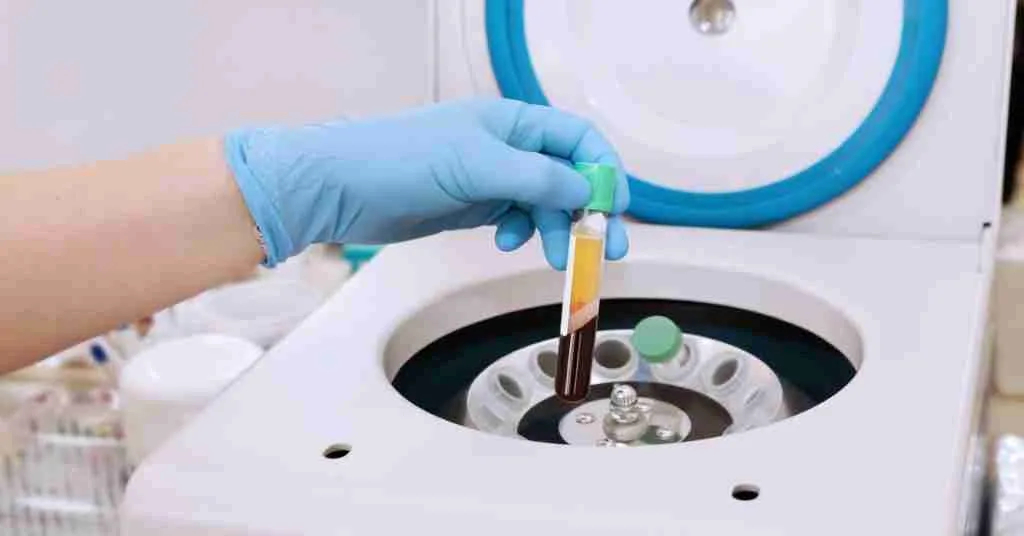
PRP is a concentrated component of a patient’s blood, enriched with platelets, growth factors, and bioactive compounds. By spinning the blood in a centrifuge, PRP is separated and prepared for injection into the injury site. Its growth factors—such as platelet-derived growth factor (PDGF), transforming growth factor-beta (TGF-β), and vascular endothelial growth factor (VEGF)—stimulate healing by promoting:
- Cell proliferation
- Angiogenesis (formation of new blood vessels)
- Extracellular matrix synthesis
These properties make PRP a valuable tool for addressing the limited healing capacity of the meniscus, particularly in areas with poor blood supply.
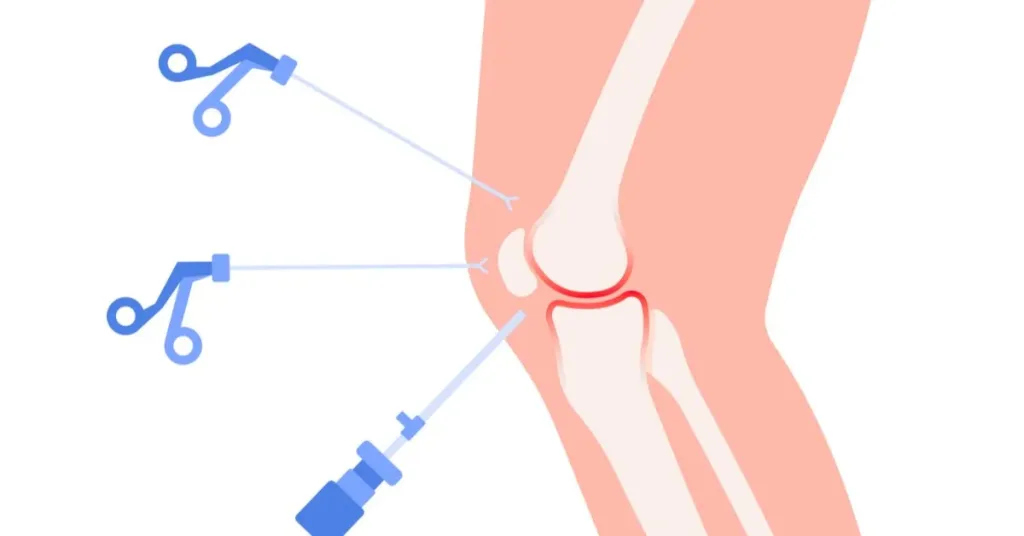
How Is PRP Used In Meniscus Repair?
PRP is typically administered during or after meniscus repair surgery. Common methods include:
- Direct Injection: PRP is injected directly into the repair site to promote healing.
- Suture Augmentation: PRP is applied around sutures to strengthen repair.
The procedure involves collecting the patient’s blood, processing it to isolate PRP, and injecting it into the targeted area under sterile conditions. Some techniques use ultrasound guidance to ensure precise placement.
Benefits Of PRP In Meniscus Repair
Evidence suggests that PRP can offer several advantages:
- Enhanced Healing: PRP’s growth factors activate meniscal cells, stimulating tissue regeneration and reducing healing time.
- Pain Reduction: Anti-inflammatory properties of PRP may alleviate pain during recovery.
- Lower Failure Rates: Studies indicate reduced rates of repair failure when PRP is used alongside traditional methods.
Evidence From Studies
Positive Outcomes
A meta-analysis by Li and Weng (2022) reviewed nine clinical studies comparing meniscus repair with and without PRP. Key findings included:
- Failure Rates: PRP-treated groups showed significantly lower failure rates (16.7%) compared to non-PRP groups (21.6%).
- Pain Relief: Improved scores on the Visual Analog Scale (VAS) for pain and the Knee Injury and Osteoarthritis Outcome Score (KOOS).
Mixed Results
Despite its promise, PRP’s benefits are not universal. Migliorini et al. (2022) found no significant improvement in patient-reported outcomes, such as the Lysholm and IKDC scores, or reduction in revision rates. This inconsistency may stem from:
- Variations in PRP preparation techniques
- Differences in patient demographics (age, injury severity)
- Lack of standardization in clinical trials.
Risks And Limitations Of PRP
While generally safe, PRP therapy has its challenges:
- Variable Efficacy: Results can differ based on preparation methods, platelet concentration, and application techniques.
- Short-Term Data: Most studies have follow-ups ranging from 6 to 24 months, leaving long-term effects unclear.
- Cost: PRP increases the cost of meniscus repair procedures, raising questions about its cost-effectiveness.
- Minimal Adverse Effects: While rare, risks include infection, pain at the injection site, or allergic reactions.
FAQs
1. What Is The Success Rate Of PRP in Meniscus Repair?
PRP has been shown to lower failure rates in meniscus repair, with studies reporting a success rate of approximately 83.3% compared to 78.4% in traditional repair methods. However, results can vary based on individual factors and preparation techniques.
2. Is Prp Treatment Painful?
The PRP injection itself may cause mild discomfort, similar to a typical injection. Most patients report minimal pain, and the anti-inflammatory properties of PRP can help reduce postoperative discomfort.
3. How Long Does It Take To See Results With Prp?
Patients may notice improvements in pain and mobility within a few weeks. However, complete healing can take several months, depending on the severity of the injury and the surgical procedure.
4. Are There Any Risks Associated With Prp?
PRP is considered safe since it uses the patient’s own blood. Rare risks include infection, allergic reactions, or localized swelling and pain at the injection site.
5. Can PRP Be Combined With Other Treatments?
Yes, PRP is often used alongside surgical techniques such as sutures and grafts to enhance healing. It can also complement rehabilitation exercises and physiotherapy for better outcomes.
Conclusion
PRP therapy is a promising adjunct in meniscus repair surgery, particularly for enhancing pain management and promoting tissue healing. However, inconsistencies in outcomes and preparation methods limit its widespread adoption. Patients and surgeons should discuss the potential benefits and risks to determine if PRP is suitable. As research advances, standardized protocols and long-term data may solidify PRP’s role in orthopedic procedures.
References
- Li Z, Weng X. Platelet-rich plasma use in meniscus repair treatment: a systematic review and meta-analysis of clinical studies. J Orthop Surg Res. 2022. doi:10.1186/s13018-022-03293-0. Available at: https://josr-online.biomedcentral.com/articles/10.1186/s13018-022-03293-0
- Utrilla GS, Degano IR, D’Ambrosi R. Efficacy of platelet-rich plasma in meniscal repair surgery: a systematic review of randomized controlled trials. J Orthop Traumatol. 2024. doi:10.1186/s10195-024-00799-7. Available at: https://jorthoptraumatol.springeropen.com/articles/10.1186/s10195-024-00799-7
- Haunschild ED, Huddleston HP, Chahla J, Gilat R, Cole BJ, Yanke AB. Platelet-rich plasma augmentation in meniscal repair surgery: a systematic review of comparative studies. Arthroscopy. 2020;36(6):1765-1774. doi:10.1016/j.arthro.2020.01.038. Available at: https://www.arthroscopyjournal.org/article/S0749-8063(20)30120-1/abstract.
- Migliorini F, Cuozzo F, Cipollaro L, Oliva F, Hildebrand F, Maffulli N. Platelet-rich plasma (PRP) augmentation does not result in more favourable outcomes in arthroscopic meniscal repair: a meta-analysis. J Orthop Traumatol. 2022. doi:10.1186/s10195-022-00630-1. Available at: https://jorthoptraumatol.springeropen.com/articles/10.1186/s10195-022-00630-1.