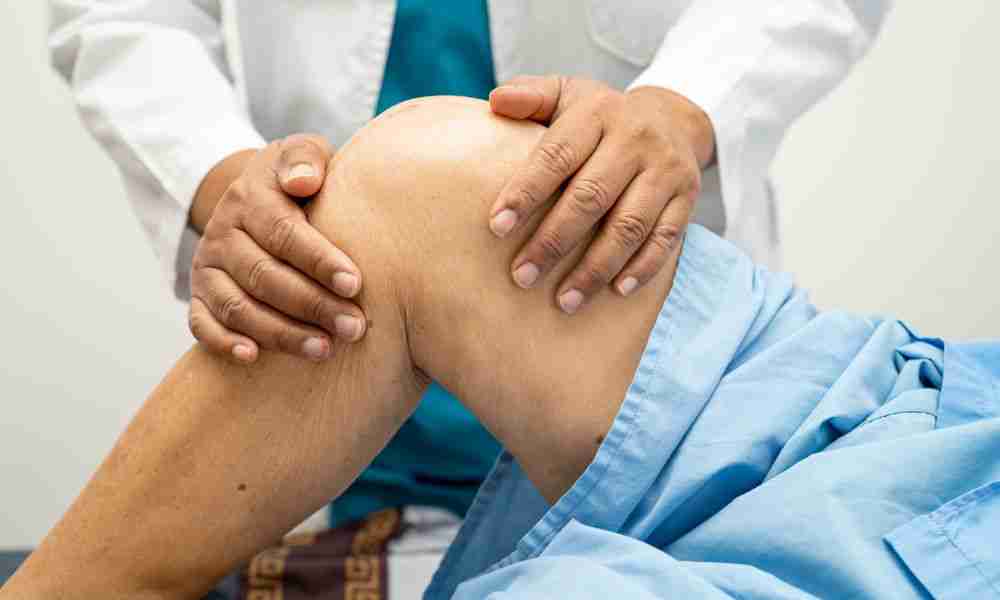
Post-traumatic arthritis results from joint injuries that lead to cartilage damage, joint instability, and chronic pain. Advanced cases often require surgical intervention to improve mobility and quality of life. This article explores the causes, treatment options, and surgical interventions for post-traumatic arthritis, offering evidence-based insights.
What Causes Post-Traumatic Arthritis?
Post-traumatic arthritis develops due to joint injuries that disrupt the normal structure and function of cartilage, bones, and surrounding tissues. Unlike osteoarthritis, which develops gradually, post-traumatic arthritis occurs after a specific traumatic event and can manifest weeks, months, or even years later. Common causes include:
Common Causes:
- Fractures within a joint: Intra-articular fractures damage cartilage and bone, creating rough surfaces that accelerate wear.
- Ligament injuries: Tears in the anterior cruciate ligament (ACL) or severe ankle sprains destabilize the joint, causing stress and cartilage damage.
- Dislocations: Joint dislocations damage cartilage and ligaments, leading to abnormal alignment and increased wear.
- Direct trauma: Hard hits or falls can cause inflammation and long-term cartilage damage.
Mechanism of Arthritis Development
- Mechanical Stress: Injuries disturb the joint’s load distribution.
- Inflammatory Response: Trauma releases cytokines, triggering cartilage breakdown.
- Structural Abnormalities: Poorly healed fractures or deformities increase joint stress and wear.
Treatment Options for Post-Traumatic Arthritis
Non-Surgical Treatments
- Physical Therapy: Strengthens muscles around the joint, improving stability.
- Medications: NSAIDs and corticosteroid injections reduce inflammation and pain.
Lifestyle Modifications
- Using braces or assistive devices.
- Avoiding high-impact activities.
Surgical Treatments
For severe cases, surgical intervention may be necessary and can include various advanced procedures.
Surgical Interventions: Key Procedures
Total Knee Arthroplasty (TKA)
This procedure replaces the damaged surfaces of the knee joint with metal and plastic components. It is typically indicated for advanced post-traumatic arthritis of the knee that results in severe pain and mobility restrictions.
- Procedure: The surgeon removes the damaged cartilage and bone from the femur, tibia, and patella, replacing them with prosthetic components.
- Benefits: Significant pain relief and improved joint function.
- Risks: Infection, loosening of the prosthesis, blood clots, and the need for revision surgery in the future.
- Recovery: Patients usually regain mobility within 3–6 months with dedicated physical therapy.
Patellofemoral Arthroplasty (PFA)
Patellofemoral arthroplasty is commonly performed in patients with a history of patella fractures, particularly when complications such as nonunions (unhealed fractures) or patellofemoral arthritis have developed.
This procedure focuses on resurfacing the damaged patellofemoral joint, relieving pain, and restoring function while preserving healthy knee structures. Preoperative planning is essential to address deformities or hardware-related challenges from prior surgeries, ensuring optimal outcomes.
- Procedure: The surgeon resurfaces the patella (kneecap) and the trochlea (groove at the end of the thigh bone) with prosthetic components.
- Benefits: Faster recovery compared to total knee replacement, preservation of healthy knee compartments, and reduced invasiveness.
- Challenges: Potential degeneration in other compartments of the knee over time, leading to additional surgeries.
- Ideal Candidates: Patients with minimal cartilage damage in other areas of the knee.
Partial Knee Replacement
This option is suitable for patients with localized arthritis affecting only one compartment of the knee.
- Procedure: The surgeon removes the damaged cartilage and bone in the affected compartment, replacing it with prosthetic components while preserving healthy cartilage, ligaments, and bone.
- Advantages: Smaller incisions, quicker recovery, and retention of natural knee motion.
- Risks: Arthritis progression in other compartments and the potential need for a future total knee replacement.
- Recovery: Generally shorter than that of a total knee replacement, with most patients resuming normal activities within weeks.
Hardware Removal
Sometimes, old hardware (such as screws, plates, or rods) must be removed before joint replacement. This step can be challenging and requires careful planning, especially when prior surgeries involve these implants.
- Procedure: Hardware removal is often performed during the same surgery as joint replacement. It requires precision to avoid damaging surrounding tissues.
- Challenges: The presence of nonunions (unhealed fractures) or malunions (healed bones with deformities) may complicate the procedure. Careful preoperative planning ensures optimal outcomes.
- Impact: Essential for the long-term success of subsequent surgical interventions.
Arthroscopy
Arthroscopy is a minimally invasive procedure for diagnosing and treating joint issues. It is often used for less severe post-traumatic arthritis cases.
- Procedure: A small camera (arthroscope) and surgical tools are inserted through small incisions to remove debris, repair minor cartilage damage, or perform debridement.
- Advantages: Less pain, faster recovery, and minimal scarring.
- Limitations: Primarily effective for early-stage arthritis or minor joint damage.
Osteotomy
This procedure, designed to realign bones and redistribute weight-bearing stress on the joint, is often used for younger patients with post-traumatic arthritis.
- Procedure: A wedge of bone is removed or added near the damaged joint, altering alignment to relieve stress on the affected area.
- Advantages: Delays the need for joint replacement and preserves natural joint tissue.
- Risks: Longer recovery period and the possibility of arthritis progression.
- Ideal Candidates: Active patients with arthritis confined to one side of the joint.
Joint Fusion (Arthrodesis)
Joint fusion is a stabilizing procedure used when other treatments fail, particularly for smaller joints like the ankle or wrist.
- Procedure: The surgeon fuses the bones of the joint together, eliminating motion but relieving pain.
- Benefits: Permanent pain relief and improved stability.
- Drawbacks: Loss of joint mobility, which may affect daily activities.
- Indications: Severe arthritis unresponsive to other surgical interventions.
Total Hip Arthroplasty (THA)
A highly effective solution for post-traumatic arthritis in the hip joint, especially in cases involving avascular necrosis or extensive cartilage damage.
- Procedure: The damaged femoral head and acetabulum are replaced with prosthetic components made of metal, ceramic, or plastic.
- Benefits: Long-lasting pain relief, improved mobility, and high success rates.
- Risks: Joint dislocation, bone loss around the implant, and the need for revision surgery over time.
- Recovery: Patients typically regain full mobility within 3–6 months, depending on adherence to rehabilitation protocols.
Conclusion
Post-traumatic arthritis is a challenging condition requiring tailored treatment strategies. Non-surgical options like physical therapy and medications provide relief for early-stage arthritis, while advanced cases benefit from surgical interventions such as total knee arthroplasty, patellofemoral arthroplasty, and total hip arthroplasty. Addressing complex factors like prior hardware or structural deformities is crucial for surgical success. Consulting with an orthopedic specialist ensures the best outcomes for long-term joint health and mobility.
References
- Kornah BA, et al. Managing of post-traumatic knee arthritis by total knee arthroplasty: case series and literature review. J Orthop Surg Res. 2019;14(168):1-9. Available from. Source
- Elkady RH, et al. Total hip replacement in post-traumatic hip arthritis in young adult patients. Am Res J Orthop Trauma. 2016;2(1):1-9. Source
- Mayo Clinic. Patellofemoral arthroplasty in arthritis patients. Orthopedic Update. 2012;6(1):1-7. Source