Regenerative Medicine in Honolulu, Hawaii: The Benefits of Orthobiologic Injections
Regenerative Medicine Expert
What Are Orthobiologics?
Orthobiologics is a type of regenerative medicine that can improve the healing of bones, muscles, tendons, and ligaments. They are made from substances that are naturally found in your body and can help you avoid major surgical procedures. Orthobiologic products contain a multitude of components including growth factors, cytokines, collagens, proteins, extracellular matrix, and hyaluronic acid.
Types Of Injuries That Can Be Treated With Orthobiologic Injections
Orthobiologic injections can help to repair a wide variety of injuries, including damage to joint cartilage from osteoarthritis; soft tissue tears as in tendonitis; or painful soft tissue conditions such as bursitis.
How Do Orthobiologic Injections Work?
Orthobiologics work by stimulating the body’s natural ability to heal itself. They do this by providing the cells with the necessary building blocks to repair or regenerate the damaged tissue. This can lead to improved healing times and reduced pain and inflammation.
What Are the Benefits of Orthobiologic Injections?
There are many benefits of orthobiologic injections including:

Why Use Orthobiologics?
There are many reasons why you might want to consider using orthobiologics. For example, if you have an injury that isn’t healing properly, orthobiologic injections can help promote healing. Additionally, orthobiologics can help you avoid surgery or other invasive procedures.
Orthobiologic injections can be an excellent option for those who want to avoid surgery or for those who have not had success with other treatments such as physical therapy or pain medication. If you are considering regenerative medicine injections, be sure to consult with a trained physician who has experience in this field.

Are There Any Risks Associated With Orthobiologic Injections?
As with any medical procedure, there are some risks associated with orthobiologic injections. However, these risks are generally rare and can include infections, bleeding, or nerve damage.
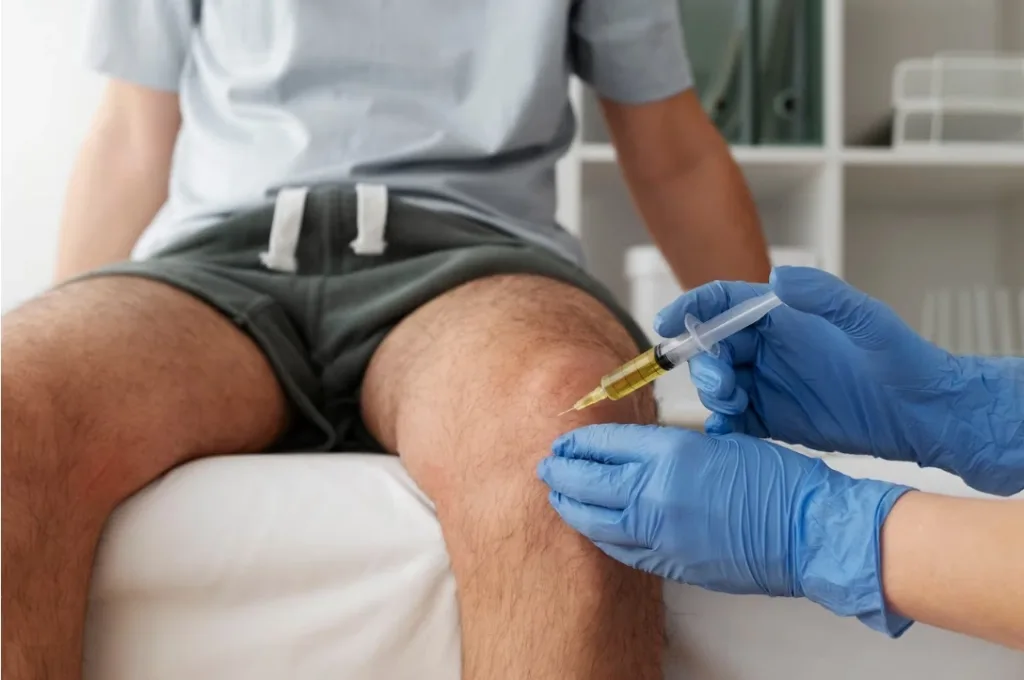
What are some common Orthobiologic Injections?
There are many different types of orthobiologic injections. Some common ones include platelet-rich plasma (PRP), hyaluronic acid (HA), bone marrow aspirate concentrate (BMAC), and amniotic tissue allografts.
Platelet Rich Plasma (PRP) is made from your own blood and contains a high concentration of platelets. Platelets are small cells that contain many growth factors that promote healing. PRP is often used to treat arthritis, tendonitis, bursitis, muscle strains, and ligament sprains.
Hyaluronic acid (HA) is a substance that is found naturally in your body. It helps to lubricate and cushion your joints. HA is often used to treat osteoarthritis.
Alpha 2 macroglobulin (A2M) is a naturally occurring protein found in blood plasma, known for its broad-spectrum protease inhibition capabilities. This protein plays a crucial role in the body’s immune system by trapping and neutralizing enzymes that break down proteins, which are often released during tissue inflammation and degeneration. A2M has gained attention for its potential in treating osteoarthritis and similar degenerative joint diseases. The mechanism involves A2M binding to and neutralizing the enzymes that degrade cartilage and other tissues, thus potentially slowing the progression of arthritis and providing pain relief.
Bone marrow aspirate concentrate (BMAC) is another type of orthobiologic injection that is made from your own bone marrow. Bone marrow contains mesenchymal stem cells and growth factors. BMAC is often used to treat arthritis or joint pain. It is also commonly used to stimulate bone growth in patients with avascular necrosis or difficulty with healing fractured bones.
Adipose-derived mesenchymal stem cells (AD-MSCs) are a type of stem cell harvested from adipose tissue, commonly known as body fat. These cells are increasingly recognized for their potential in regenerative medicine due to their ability to differentiate into various cell types, including bone, cartilage, and muscle cells. AD-MSCs are particularly valuable because adipose tissue is abundant and can be harvested with minimally invasive techniques, making it a less painful and more efficient source compared to bone marrow extraction.
Amniotic tissue allografts (stem cells) are derived from donor tissue and contain a high concentration of growth factors and proteins that help promote healing. Amniotic tissue allografts are often used to treat chronic wounds or skin ulcers.

Dr. Morton’s Protocol
Our approach to managing musculoskeletal discomfort with a personalized care plan that leverages regenerative medicine techniques, including PRP (Platelet-Rich Plasma) injections and laser therapy, alongside hyaluronic acid injections, is comprehensive and innovative. Here’s an outline to further refine and support this protocol, emphasizing patient care and maximizing outcomes:
Initial Assessment
Office Examination: Begin with a hands-on evaluation to assess the patient’s condition, focusing on identifying the specific sources of discomfort and any functional limitations.
Review of Imaging: Require up-to-date imaging studies (e.g., x-ray, MRI, ultrasound) to visualize the internal structure of the knee, aiding in precise diagnosis and treatment planning.
Treatment Plan Overview
Initial PRP or BMAC Injection:
Aim: Reduce inflammation and decelerate tissue degeneration.
Process: Extract PRP from the patient’s blood, ensuring a natural treatment method without foreign substances. We may choose a PRP or BMAC injection that contains A2M for the first injection
Laser Therapy Sessions:
Schedule: 10 -12 sessions over six weeks.
Purpose: Enhance blood flow and diminish inflammation, supporting tissue healing.
Subsequent PRP Injections:
Schedule: Two additional injections during the six-week period.
Goal: Supply growth factors to foster the regeneration of healthy tissue.
Hyaluronic Acid Injection:
Timing: Offered during the initial six-week treatment phase.
Function: Lubricate the knee joint and improve mobility, complementing PRP’s regenerative effects.
Six-Month Follow-Up
Repeat PRP and Hyaluronic Acid Injection
Administer a repeat PRP injection simultaneously with hyaluronic acid to further encourage tissue growth and repair by increasing healthy proteins in the knee while sustaining joint lubrication.
Ongoing Care and Adjustments
Rehabilitation and Physical Therapy: Integrate tailored exercises and therapies to strengthen the knee, improve range of motion, and support recovery throughout the treatment period.
Lifestyle Adjustments and Nutrition: Advice on dietary and lifestyle habits supporting joint health and overall well-being.
Monitoring and Evaluation: Schedule regular follow-ups to assess progress, adjust treatments as needed, and ensure the knee is healing optimally.
This comprehensive care plan offers a holistic and patient-centric approach to knee discomfort, leveraging the latest regenerative medicine while ensuring personalized care tailored to each patient’s unique needs and circumstances.

Enhancing PRP Therapy with Hyaluronic Acid Gel Injections
Building on the success of our Platelet-Rich Plasma (PRP) Therapy, we now offer an advanced treatment option that includes the addition of Hyaluronic Acid (HA) Gel Injections, also known as viscosupplementation. This innovative combination is designed to provide a dual-action approach to treating orthopedic conditions, leveraging the regenerative properties of PRP and the lubricating benefits of HA for enhanced patient outcomes.
Synergistic Benefits
Enhanced Healing: The growth factors in PRP can help to stimulate the repair of damaged tissues. At the same time, HA can improve joint function and reduce friction, potentially allowing for a better healing environment.
Increased Effectiveness: Some studies suggest combining PRP and HA could be more effective than either treatment alone, especially in osteoarthritis treatment. This is likely because PRP can enhance the viscoelastic properties of HA, thus improving its effectiveness.
Reduced Inflammation: Both PRP and HA have anti-inflammatory properties. PRP reduces inflammation by releasing growth factors that modulate the inflammatory response, while HA can directly reduce inflammation in the joint. Together, they may provide a more potent anti-inflammatory effect.
Synergistic Action: HA provides immediate relief by improving the joint’s mechanical function, while PRP’s effects are more gradual, focusing on long-term healing and tissue regeneration. This synergistic action can provide both immediate symptom relief and longer-term benefits.
Insurance Coverage for Hyaluronic Acid Injections
Understanding the financial aspects of healthcare is crucial for our patients. Here’s how we address insurance coverage for HA Gel Injections:
Insurance Authorization Assistance: We help you obtain insurance authorization for HA Gel Injections when your plan covers them. Coverage for HA injections can vary, often depending on the diagnosis and your specific insurance policy.
Transparent Communication: Before proceeding with the combined treatment, we will go over your insurance benefits to determine coverage eligibility for HA injections. We want you to know that we are committed to transparency and will provide detailed information regarding potential out-of-pocket costs.
Dedicated Support: Our team is here to guide you through the insurance verification process, helping you understand your coverage options and any necessary steps to secure authorization for HA Gel Injections.

Synergy of Laser Therapy and PRP Injections
The integration of MLS (Multiwave Locked System) robotic laser therapy with Platelet-Rich Plasma (PRP) injections represents a cutting-edge approach to enhance the healing process through advanced therapeutic mechanisms. MLS laser therapy utilizes specific wavelengths of light in a controlled, robotic manner to precisely target affected tissues, offering distinct advantages in reducing inflammation, alleviating pain, and accelerating tissue repair. Here’s how MLS robotic laser therapy can complement and amplify the healing effects of PRP injections:
1. Enhanced Cellular Activity and Regeneration
Targeted Mitochondrial Activation: MLS robotic laser therapy precisely stimulates mitochondrial activity in targeted cells, leading to an increased production of adenosine triphosphate (ATP), the cell’s energy currency. This boost in cellular energy enhances metabolism and promotes faster regeneration of damaged tissues.
Growth Factor Stimulation: PRP injections deliver a high concentration of growth factors essential for tissue repair. The precise application of MLS laser therapy can further enhance the activity of these growth factors, optimizing the regenerative process initiated by PRP.
2. Reduced Inflammation
Modulation of Inflammatory Mediators: The MLS robotic laser can precisely modulate the levels of inflammatory mediators, reducing inflammation more efficiently than PRP alone. This targeted approach leads to a quicker reduction in swelling and pain, creating a conducive environment for healing.
Enhanced Lymphatic Drainage: The robotic precision of MLS laser therapy promotes effective lymphatic drainage, aiding in the reduction of edema and being beneficial for post-PRP injection healing.
3. Improved Blood Circulation
Stimulated circulation: The MLS robotic laser’s ability to improve blood circulation to the treated area. Enhanced blood flow ensures the delivery of more oxygen and nutrients, which are crucial for tissue repair, and synergizes with the growth factors provided by PRP.
4. Pain Reduction
Analgesic Effect: MLS robotic laser therapy achieves analgesic effects by reducing inflammation, inhibiting pain transmission in nerve fibers, and triggering the release of endorphins. This results in immediate pain relief post-PRP injections, enhancing patient comfort throughout the healing process.
5. Accelerated Tissue Repair
Collagen Production: The combination of PRP and MLS laser therapy stimulates collagen synthesis, which is essential for the strength and elasticity of connective tissues. The synergistic effect of these treatments can lead to more robust and quicker tissue repair.
Integrating MLS robotic laser therapy with PRP injections takes advantage of both treatments’ precision, control, and advanced therapeutic effects, potentially leading to an enhanced and more efficient healing process. This innovative combination is especially beneficial for treating orthopedic conditions, sports injuries, and other scenarios where accelerated tissue repair is desired, leveraging the latest advancements in medical technology to improve patient outcomes.

Are regenerative Medicine Injections Covered by Insurance?
Orthobiologic injections are often not covered by insurance. However, some insurance companies may cover certain types of orthobiologic injections, such as HA, if used to treat a specific diagnosis such as osteoarthritis. It is important to check with your insurance company to see if they will cover the cost of your procedure
Why Orthopedic Surgeons Are the Preferred Choice for Regenerative Medicine Injections
Choosing an orthopedic surgeon for injection therapy, especially for musculoskeletal conditions, offers several advantages over chiropractors or non-musculoskeletal physicians due to their specialized training, extensive knowledge of musculoskeletal anatomy and pathology, and surgical expertise. Here are key reasons why an orthopedic surgeon might be the preferred choice:
1. Specialized Musculoskeletal Knowledge
Deep Understanding: Orthopedic surgeons possess a profound understanding of the musculoskeletal system, including bones, muscles, ligaments, tendons, and joints. This specialized knowledge is crucial for accurately diagnosing conditions and determining the most effective injection sites and techniques.
Condition-Specific Experience: They have experience treating various musculoskeletal conditions, from sports injuries to degenerative diseases, giving them a broad perspective on managing these issues with injection therapy.
2. Advanced Diagnostic Skills
Accurate Diagnosis: Orthopedic surgeons are trained to use advanced diagnostic tools, such as MRI, CT scans, and ultrasound, which aid in making precise diagnoses and planning treatment. This capability ensures that the injection targets the root cause of the problem.
Guided Injection Techniques: They often employ imaging guidance (e.g., ultrasound-guided injections) to enhance the precision of the injection, improving its effectiveness and reducing the risk of complications.
3. Comprehensive Treatment Options
Integrated Care: Orthopedic surgeons can offer a comprehensive treatment plan beyond injections, including surgery, physical therapy, and medication management. This integrated approach ensures a holistic treatment strategy tailored to patients’ needs.
Surgical Expertise: In cases where injections are part of a broader treatment plan that might include surgery, an orthopedic surgeon overseeing the care ensures continuity and understanding of the overall treatment goals.
4. Specialized Injection Procedures
Wide Range of Injections: Orthopedic surgeons are equipped to perform various specialized injection procedures, such as corticosteroid injections for inflammation, viscosupplementation for osteoarthritis, and regenerative medicine injections like PRP or stem cells. Their expertise ensures that patients receive the most appropriate type of injection for their condition.
5. Safety and Efficacy
Minimized Risk of Complications: The extensive training and experience of orthopedic surgeons in performing injections reduce the risk of complications, such as infection or damage to surrounding tissues.
Evidence-Based Practice: Orthopedic surgeons rely on the latest evidence-based practices to ensure that the treatments they offer, including injections, are supported by the latest research and clinical guidelines, maximizing safety and effectiveness.
While chiropractors and non-musculoskeletal physicians have their areas of expertise, they may need the specialized training or focus on musculoskeletal conditions that orthopedic surgeons do. Non-musculoskeletal physicians, including those specializing in internal medicine, family medicine, or other non-orthopedic specialties, may not have the detailed anatomical knowledge, precision, or the ability to integrate injection treatments into a broader orthopedic care plan like an orthopedic surgeon. An orthopedic surgeon is generally the most qualified professional to administer such therapy for musculoskeletal injections, particularly those requiring detailed anatomical knowledge and precision and the ability to integrate these treatments into a comprehensive care strategy.
Conclusion:
Orthobiologic injections are a type of regenerative medicine that can offer many benefits to patients. They are made from substances that are naturally found in your body and can help you avoid major surgical procedures. Orthobiologic injections can be an excellent option for those who want to avoid surgery or for those who have not had success with other treatments such as physical therapy or pain medication.
If you are considering regenerative medicine injections, be sure to consult with a trained physician who has experience in this field. Dr. Morton and his team are your premier source for orthobiologic injections in Hawaii. He has extensive experience in treating a variety of injuries and conditions with these injections. Contact his office today to schedule a consultation and learn more about the benefits of orthobiologic injections.