Avascular Necrosis of the Hip
Content
How does Avascular Necrosis (AVN) of the Hip Occur?
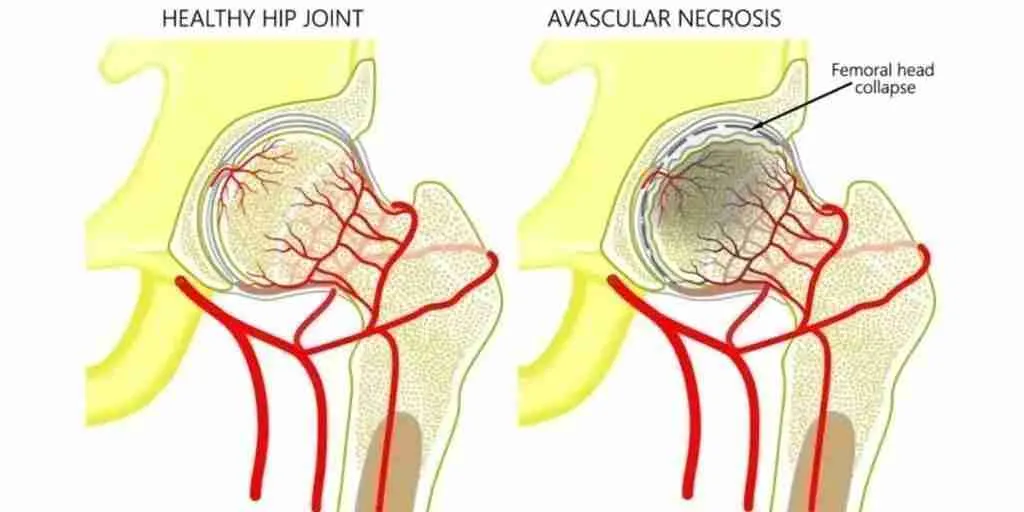
What Causes AVN?
As stated above, avascular necrosis has many causes. In fact, most researchers believe that the condition is caused by a constellation of factors acting at once to create the perfect storm. This condition can occur in children or adults and can be caused by medications, conditions, or other factors.
Two common causes that cause avascular necrosis are glucocorticoids and alcohol. Glucocorticoids, commonly known as steroids, are used to treat many medical conditions. In some people, they can impair blood flow to the femoral head and cause necrosis of the bone. Excessive alcohol use also causes avascular necrosis. Scientists believe this is due to changes in stress levels, an increase in fat, and sluggish blood flow.
Many medical conditions are associated with avascular necrosis of the hip. These include Lupus, the presence of antiphospholipid antibodies, Sickle Cell Disease, Gaucher Disease, Decompression Disease, Acute Lymphoblastic Leukemia, and kidney transplants. Avascular necrosis in children can be due to a congenital condition called Legg-Calvé-Perthes disease. Additionally, trauma, such as falling or being hit by a car, puts both adults and children at risk for avascular necrosis.
Determining the Stage of Avascular Necrosis of the Hip
Identifying the stage of avascular necrosis (AVN) of the hip is crucial for selecting the most effective treatment. Let’s explore how healthcare professionals arrive at this important determination.
Evaluation and Examination
The process begins with a detailed assessment that includes the following steps:
Symptom Assessment: Doctors will inquire about your symptoms, focusing on their onset and progression. Understanding whether your pain has increased over time provides valuable context.
Medical History Review: Your medical history is thoroughly examined for any risk factors such as previous hip injuries, corticosteroid usage, or underlying conditions associated with AVN.
Physical Examination: This involves testing the mobility of your hip to identify positions that trigger discomfort or pain. This hands-on approach helps doctors gather critical information about your hip’s condition.
Imaging and Testing
To confirm AVN and determine its stage, various tests are conducted:
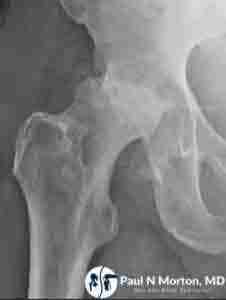
X-rays: Provide a basic view of your hip structure, revealing changes in bone density and shape.
MRI Scans: Offer a more detailed image, highlighting any early damage to bone and tissues not visible on X-rays.
Additional Diagnostics
Blood Tests: While not directly indicating the AVN stage, these tests are useful for identifying potential underlying causes or contributing factors.
Understanding the Stage
Once all information is gathered, doctors establish whether the condition is in its early, middle, or late stages. Each stage reflects different levels of bone and joint damage and guides the appropriate treatment strategy. Early stages might focus more on non-invasive interventions, while advanced stages could require surgical options.
By following this comprehensive evaluation process, healthcare providers ensure a targeted and effective approach to managing avascular necrosis of the hip.
What are my Treatment Options for Avascular Necrosis of the Hip?
Avascular necrosis can be difficult to treat depending on the patient. The first step is to identify the cause of the necrosis and stop or manage the offending agent. This also includes optimizing other risk factors that impede blood flow, including smoking. Early in the disease, some physicians recommend starting with non-operative management. Non-operative management includes reducing weight-bearing by using crutches and using medications to reduce pain and maintain bone density. However, non-operative management has been found to be ineffective at halting the progression of the disease. Therefore, many people turn to operative management.
Operative management can be divided into two classes: joint-preserving procedures and joint replacement procedures. One option for a joint-preserving procedure is called core decompression. This is when the surgeon uses a tool to decompress the femoral head to restore blood flow. They often then use a bone graft to fill in the parts of the bone that have died.
Researchers have examined the success rate of core decompression with and without bone grafting have mixed results. Many studies have demonstrated that patients have significant pain relief with core decompression. Only certain patients reported excellent outcomes from core decompression, particularly those that had the procedure done early in the disease before the bone collapsed. Other patients had less success.
Core decompression surgery, when enhanced with stem cell (Bone Marrow Aspirate Concentration) injection, has shown improved outcomes relative to the procedure by itself. Patients often experience greater reductions in hip pain and enhanced joint function. The addition of stem cells plays a crucial role in slowing the progression of avascular necrosis (AVN), thereby significantly lowering the risk of the femoral head collapsing. As a result, the likelihood that a patient will require total hip replacement surgery is minimized.
When joint-preserving procedures are not successful, the next option is a joint replacement. Total hip replacements are generally successful with a low revision rate. Because the revision rate is low, some surgeons prefer total hip replacements over joint-preserving procedures. Other surgeons prefer to be more selective with who receives a total hip replacement depending on their disease progress and lifestyle.
Factors Influencing the Prognosis of Avascular Necrosis of the Hip
The prognosis for individuals with avascular necrosis (AVN) of the hip can be influenced by several key factors:
- Underlying Cause: The root cause of AVN plays a crucial role. Whether the condition stems from trauma, steroid use, or other systemic diseases can impact treatment effectiveness and outcomes.
- Stage at Diagnosis: Early detection and intervention often lead to better outcomes. Treatment is generally more successful when AVN is diagnosed before significant bone damage occurs.
- Specific Area Affected: The location on the femoral head that is affected by necrosis affects recovery prospects. Damage to critical areas of the femoral head may lead to more complex treatment challenges.
- Patient Demographics:
- Age: Younger patients often have a more favorable prognosis as they tend to recover more efficiently.
- General Health: Overall health and lifestyle choices, including physical activity levels, can significantly affect healing and rehabilitation.
- Treatment Approach: The chosen medical or surgical intervention can significantly influence the long-term outcome.
To optimize the prognosis, it is essential for patients to maintain a healthy lifestyle and follow medical advice promptly.
Understanding the Stem Cell Implantation Procedure for Avascular Necrosis of the Hip
Stem cell implantation for avascular necrosis (AVN) of the hip is a sophisticated medical procedure designed to alleviate hip joint issues by regenerating bone with the patient’s own stem cells. Here’s an overview of what’s involved in this procedure:
Bone Marrow Collection
The journey begins with the collection of bone marrow from the patient’s iliac crest, a part of the pelvis. A needle is used to extract the marrow, which is then placed in tubes for further processing. These tubes are spun in a centrifuge to separate stem cells from other marrow components.
Core Decompression Procedure
After harvesting the stem cells, the surgeon performs a core decompression. Utilizing advanced imaging, such as a CT scan, they create a three-dimensional model of the hip joint. This model helps identify the exact regions of the femoral head affected by AVN.
Surgical Process
Through a small incisions near the hip joint—each roughly a centimeter long—the surgeon places the guide into the femoral head. This guides a precisely navigated drill to remove the necrotic bone. Once the affected bone is cleared, the surgeon injects the harvested stem cells into those areas, along with a bone graft to aid in healing.
Recovery and Aftercare
Typically, this procedure is outpatient, allowing patients to return home the same day. For those with significant pain, a short hospital stay may be required. Post-surgery, weight-bearing on the hip is possible but may require support, such as crutches or a walker, for around two weeks.
Pain management is crucial after surgery, with medications prescribed not only to alleviate discomfort but also to minimize blood clot risks.
Follow-up and Complications
Patients are encouraged to resume most regular activities after being toe touch weight bearing for weeks, but regular follow-up appointments are essential for monitoring healing progress. While complications are rare, they can include infection, bleeding, and pain at the marrow extraction site. More serious issues, such as bone fractures, blood clots, or cartilage damage, may also arise but are less common.
This procedure’s innovative approach leverages the body’s natural healing processes to fight AVN, offering many a promising return to normal activities and improved quality of life.
Understanding Stem Cells and Their Role in Treating Avascular Necrosis
Stem cells are extraordinary cells with the remarkable ability to transform into various specialized cells within the body, performing crucial functions. These cells broadly fall into two categories:
Embryonic Stem Cells: Found in embryos, these cells possess the potential to become any type of cell within the body.
Adult or Somatic Stem Cells: Located in tissues and organs like bone marrow, these cells primarily aid in the body’s natural repair processes.
When it comes to addressing avascular necrosis (AVN), adult stem cells are particularly significant. This condition involves the loss of blood flow to the bone, causing tissue death. Here’s how stem cells are employed to combat AVN:
Collection: Stem cells are harvested from the patient’s own bone marrow. This method not only enhances compatibility but also reduces the risk of rejection.
Transplantation: The collected cells are strategically transplanted into the damaged areas of the femoral head, which is the upper part of the thigh bone affected by AVN.
Regeneration: Once in place, these stem cells differentiate into bone cells. The new cells work to remove the necrotic, or dead, bone, facilitating the replacement with healthy, robust bone tissue.
This innovative use of stem cells not only addresses the immediate damage caused by AVN but also encourages long-term healing and functionality. Through targeted regeneration, patients can experience improvements in mobility and a reduction in pain, illustrating the transformative potential of stem cell therapy.
Conclusion
Avascular necrosis of the hip is a condition that causes pain and reduced mobility of the hip. Treatment is complicated and depends on the patient, his or her lifestyle, and his or her risk factors. If you suffer from avascular necrosis of the hip, schedule an appointment to talk with Dr. Morton to determine the best course of action for you.
Frequently Asked Questions About Avascular Necrosis (FAQ)
Long-distance travel should usually be avoided until at least after your initial post-operative visit with your surgeon. The concern with long-distance travel is the possibility of the development of a blood clot, or missing a postoperative complication.
Once you are on a long trip, Dr. Morton recommends that you get up to stretch or walk at least once per hour during a long trip. Taking 81mg of aspirin daily is a useful adjunct. Dr. Morton recommends starting aspirin 2 days before your trip, and 2 days after your trip to avoid blood clots. You may want to talk with your primary care physician if you have a history of stomach ulcers, allergies, blood clots, or bleeding disorders. Usually, patients will desire an aisle seat or a lay-flat seat for long distances during their initial recovery.
The answer varies from patient to patient, and whether you have surgery on the right leg or the left leg. As a general rule, you cannot drive if you are on narcotics or unsafe on the road. Patients on average are able to return to driving between 2 and 6 weeks after surgery. I usually advise my patients that if they feel like they wouldn’t be able to stop in the event of an emergency or if a pedestrian suddenly decided to cross the road in front of the car, they should not drive. Practice on a parking lot before driving on the road.
This is a complex question depending on what job type you are doing.
Desk job: I tell most patients that they will feel well enough to begin working around two weeks after surgery. Some patients who are gung-ho will even start working immediately after surgery.
Light Labor: Light labor that requires frequent walking or light lifting. Some patients may require 6 weeks to 3 months before returning to work. Close monitoring will be needed to help you determine when you are safe.
Heavy labor: Construction and other types of manual labor usually requires at least 3 months of recovery. Some patients will have to change their careers depending on their demands. Talk with your surgeon before returning to work.
Tobacco use is known to be a significant risk factor for loosening, infection, or wound healing problems. Minimizing your tobacco use or quitting before surgery will make a significant impact. If you are able to quit for life, you will significantly reduce your risk of other complications to your overall health as well. Learn more about tobacco effects on joint replacements here.
The arthritic pain from before surgery is usually removed following hip replacements. Many patients tell me they have minimal to no pain following surgery initially. Some patients have soreness for up to 2 months. Again, I have noticed that many patients have a lower amount of pain through the anterior approach.
Hip replacement recovery is variable. Many patients are feeling good at 6 weeks. It may take 3 months to a year before you completely recover from your hip replacement. The anterior hip replacement consistently allows for a quicker recovery.
50% of people who are diagnosed with AVN of the hip undergo surgery within 3 years of their diagnosis. If there is bone collapse, this process occurs sooner.
Related Pages
Personalized Alignment In Knee Replacement Surgery
Discover how personalized alignment in knee replacement surgery tailors the procedure to your unique anatomy for better outcomes, faster recovery, and improved mobility.
Hiking After Knee Replacement: Tips for Staying Active
Can you hike after a knee replacement? Yes! Discover essential recovery milestones, recommended gear, and exercises to help you safely return to the trails and stay active.
Uncemented Knee Replacement: What Patients Should Know
Uncemented knee replacement offers biological fixation for long-term durability. Discover the benefits for younger, active patients and how it compares to traditional cemented surgery.
How Much Does A Hip Or Knee Replacement Cost?
Understanding Your Expected Bills Hip or knee replacement surgery is a transformative procedure that can significantly improve the quality of life for individuals with severe arthritis or joint damage. However, the financial aspect [...]
Cost of Total Knee Replacement in Hawaii for Medicare Patients: How to Save Money with Outpatient Surgery Centers
Total knee replacement (TKA) is a life-changing procedure for patients suffering from severe arthritis or knee dysfunction. With advancements in surgical techniques, many TKAs are now performed on an outpatient basis, allowing patients to [...]
Understanding Post-Traumatic Arthritis After ACL Reconstruction
Anterior Cruciate Ligament (ACL) injuries are a common occurrence, especially among athletes and physically active individuals. While ACL reconstruction is a widely accepted procedure to restore knee stability and function, it is important to [...]