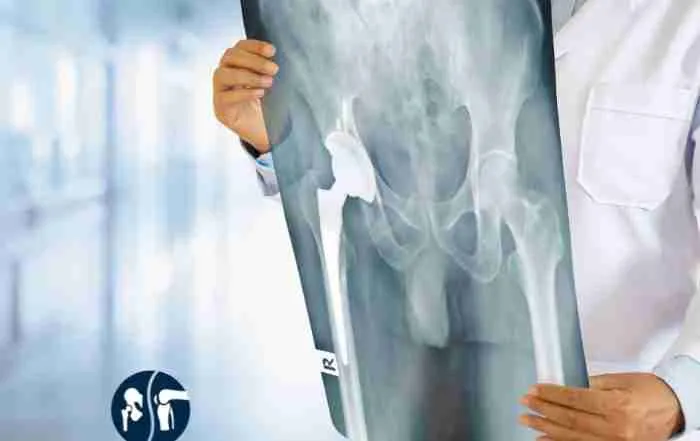
Talk with Your Hip Expert Today!
Anterior Approach Improves Hip Replacement Surgery
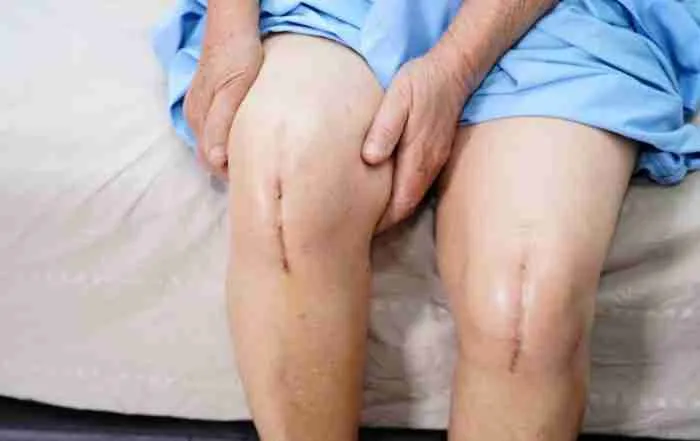
- Soft Tissue Sparing – Anterior approach avoids cutting the muscle, as it follows the natural path between the muscles.
- Smaller Incisions – Anterior approach to the hip is much closer to the hip joint, allowing for a smaller incision.
- Less Pain – Many patients do complain of pain on the day of surgery, and may not require more than Tylenol for pain control.
- No Posterior Hip Precautions – The traditional approaches require patients to avoid internally rotating the hip, or bending the hip past 90 degrees. This can be very limiting for patients during their recovery phase.
- Faster and Easier Recovery – Without posterior hip precautions and less pain after surgery, recovery is much faster
- Early Discharge From Hospital – Many patients are able to go home on the day of surgery
- Lower Risk of Hip Dislocation – More accurate positioning of implants during surgery allow for a lower risk of hip dislocation
- Equal Leg Lengths – Leg length discrepancy after surgery, especially in Hawaii (where people wear slippers or walk barefoot on the beach), can be a big deal. Intra-operative x-rays performed during the anterior hip surgery allow for more accurate placement of implants and avoid leg length issues.
Dr. Morton is an expert hip surgeon who is fellowship-trained in hip replacement surgery. Talk with him today about your hip problems!

Hip Replacement
Hip replacements involve the removal of the arthritic part of the hip. This means that the hip socket on the pelvis is resurfaced with metal, and the arthritic femoral head is removed and replaced with a ball and stem that is placed into the femur (thigh bone). There are many different approaches to the hip. The most common ways to approach the hip socket are through the posterior and anterior hip approaches

Posterior Total Hip Replacement
The traditional posterior surgical approach to total hip replacement goes through the back of the hip. This approach uses a single, long incision to get access to the hip joint. This incision cuts through the gluteus maximus muscle. The posterior hip replacement also requires the release of a small muscle group called the “short external rotators”. These muscles are important to the stability of your hip.
How is the Anterior Hip Different?
The anterior total hip arthroplasty works through an incision through the front of your thigh. This incision is performed through a muscle-sparing approach. The approach does not cut any muscle, moving apart the muscle to get access to the hip joint. Specifically, the anterior approach is between the sartorius and iliotibial band muscles. The “short external rotator muscles” are not released, meaning that the hip is more stable. The anterior approach may not be suitable for all patients. Your orthopedic surgeon will discuss different surgical approaches with you.
What are the 8 Benefits of an Anterior Hip Replacement?
- Soft Tissue Sparing – Anterior approach avoids cutting the muscle, as it follows the natural path between the muscles.
- Smaller Incisions – Anterior approach to the hip is much closer to the hip joint, allowing for a smaller incision.
- Less Pain – Many patients do complain of pain on the day of surgery, and may not require more than Tylenol for pain control.
- No Posterior Hip Precautions – The traditional approaches require patients to avoid internally rotating the hip, or bending the hip past 90 degrees. This can be very limiting for patients during their recovery phase.
- Faster and Easier Recovery – Without posterior hip precautions and less pain after surgery, recovery is much faster
- Early Discharge From Hospital – Many patients are able to go home on the day of surgery
- Lower Risk of Hip Dislocation – More accurate positioning of implants during surgery allow for a lower risk of hip dislocation
- Equal Leg Lengths – Leg length discrepancy after surgery, especially in Hawaii (where people wear slippers or walk barefoot on the beach), can be a big deal. Intra-operative x-rays performed during the anterior hip surgery allow for more accurate placement of implants and avoid leg length issues.
When should You Consider having a Hip Replacement?
A hip replacement is a good option for patients who have severe pain in their hip secondary to arthritis. Most patients with arthritis experience pain in their groin region. Sometimes this pain can be felt on the outside of their hip. Often times patients experience this pain as “knee pain”. It can often be difficult to tell when patients have pain that comes from their knee or their hip. Dr. Morton uses a combination of x-rays, physical exam, and diagnostic injections to help you determine what is contributing to your pain.
You should consider having a hip replacement when your hip causes enough pain that prevents you from enjoying your life and you have failed nonoperative treatment.
Are you a candidate for an Anterior Hip Replacement?
In general, most patients may undergo hip replacement from both approaches. The anterior total hip surgery is less suitable for patients who are overweight or have already undergone other hip surgeries in the past. Patients who have a significant deformity of the hip joint or with health problems that may slow wound healing may also be at high risk for poorer outcomes with the anterior total hip replacement. Call Dr. Morton to set up an appointment if you would like to see if you are a candidate for the anterior hip replacement.
How do you get leg length measurement right during surgery?
Traditionally, many patients after the posterior total hip replacement complained of leg length inequality and pain to the outside of their hip. Dr. Morton uses specialized tools such as x-ray during surgery to check leg-lengths intra-operatively. Sometimes getting your leg lengths perfect can be harder to achieve during revision and deformity surgery.
During surgery, Dr. Morton also considers the offset of your hip. Offset is the measurement of how far your femur bone is from your pelvis bone. The further away it is, the higher the offset. A high offset can sometimes put increased pressure on the hip and cause pain. A low offset can cause an unstable hip. Dr. Morton uses specialized tools to help figure out the appropriate offset of your hip. Talk with Dr. Morton about leg lengths and offset to understand how he will personalize placing your hip implant.
Have Realistic Expectations
When deciding to have a hip replacement, you need to understand the limitations of your joint replacement surgery. Over 90% of people who have a total hip replacement have an incredible reduction in their hip pain and a dramatic improvement in returning to a better function. For most patients with normal use and activity, the hip replacement rarely wears out the plastic spacer. Dr. Morton likes to follow-up his patients on an annual basis with an x-ray to ensure that your hip replacement is continuing to function at the best of its ability. Increased activity or weight may speed up the wear and tear on your plastic components and may cause the hip replacement to loosen or become painful. After your recovery, you will feel like you can do many physical activities. The American Academy of Orthopaedic Surgeons advises our patients to avoid running, jogging, jumping or other high-impact activities with a hip replacement.
Talk with Dr. Morton About Hip Replacement
Dr. Morton is one of the few orthopedic surgeons in Honolulu, Hawaii who is fellowship-trained in hip and knee reconstruction. He regularly takes care of complicated hip replacements, performs anterior total hip replacements, and revision total hip replacements. He performs surgery at Queen’s Medical Center which has received Advanced Certification for total hip and total knee replacement from the Joint Commission and is the only hospital in the state of Hawaii that is rated as “High Performing” in both Hip and Knee replacements by US News. If you are suffering from hip pain, schedule an evaluation today!

Frequently Asked Questions about Hip Replacements (FAQ)
Long-distance travel should usually be avoided until at least after your initial post-operative visit with your surgeon. The concern with long-distance travel is the possibility of the development of a blood clot, or missing a postoperative complication.
Once you are on a long trip, Dr. Morton recommends that you get up to stretch or walk at least once per hour during a long trip. Taking 81mg of aspirin daily is a useful adjunct. Dr. Morton recommends starting aspirin 2 days before your trip, and 2 days after your trip to avoid blood clots. You may want to talk with your primary care physician if you have a history of stomach ulcers, allergies, blood clots, or bleeding disorders. Usually, patients will desire an aisle seat or a lay-flat seat for long distances during their initial recovery.
The answer varies from patient to patient, and whether you have surgery on the right leg or the left leg. As a general rule, you cannot drive if you are on narcotics or unsafe on the road. Patients on average are able to return to driving between 2 and 6 weeks after surgery. I usually advise my patients that if they feel like they wouldn’t be able to stop in the event of an emergency or if a pedestrian suddenly decided to cross the road in front of the car, they should not drive. Practice on a parking lot before driving on the road.
This is a complex question depending on what job type you are doing.
Desk job: I tell most patients that they will feel well enough to begin working around two weeks after surgery. Some patients who are gung-ho will even start working immediately after surgery.
Light Labor: Light labor that requires frequent walking or light lifting. Some patients may require 6 weeks to 3 months before returning to work. Close monitoring will be needed to help you determine when you are safe.
Heavy labor: Construction and other types of manual labor usually requires at least 3 months of recovery. Some patients will have to change their careers depending on their demands. Talk with your surgeon before returning to work.
Tobacco use is known to be a significant risk factor for loosening, infection, or wound healing problems. Minimizing your tobacco use or quitting before surgery will make a significant impact. If you are able to quit for life, you will significantly reduce your risk of other complications to your overall health as well. Learn more about tobacco effects on joint replacements here.
The arthritic pain from before surgery is usually removed following hip replacements. Many patients tell me they have minimal to no pain following surgery initially. Some patients have soreness for up to 2 months. Again, I have noticed that many patients have a lower amount of pain through the anterior approach.
Hip replacement recovery is variable. Many patients are feeling good at 6 weeks. It may take 3 months to a year before you completely recover from your hip replacement. The anterior hip replacement consistently allows for a quicker recovery.