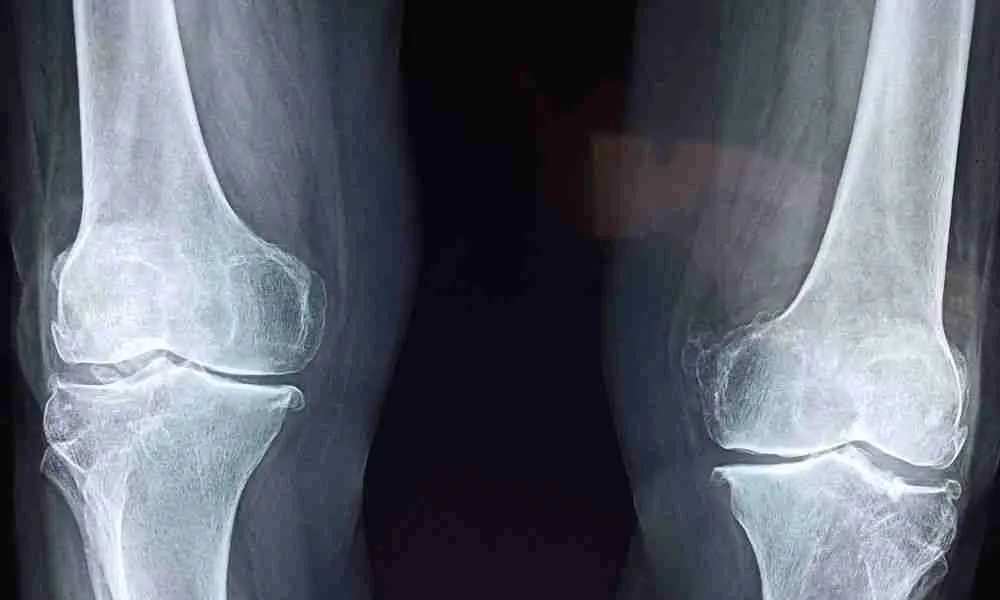
Knee arthritis, a degenerative joint condition, affects millions worldwide, reducing mobility and quality of life. As patients explore alternatives to traditional treatments, Platelet-Rich Plasma (PRP) therapy has gained traction as a promising intervention. This blog delves into the nuances of PRP for knee arthritis, including its success rates, what patients should know, and what they can expect from this innovative treatment.
Overview of PRP
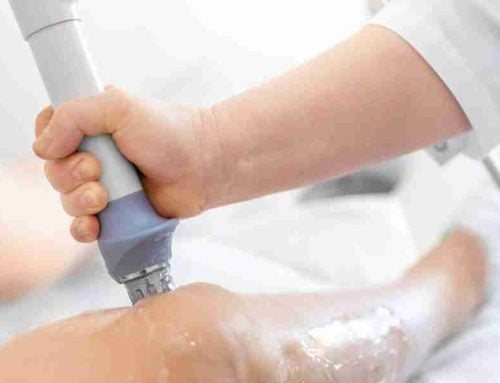
Platelet-Rich Plasma (PRP) therapy is a minimally invasive procedure derived from the patient’s blood. The process involves extracting a small amount of blood, centrifuging it to concentrate the platelets, and injecting the PRP into the affected knee joint. These platelets contain growth factors and bioactive proteins that promote tissue regeneration and healing, making PRP a natural and autologous option.
How PRP Works
- Extraction and Processing: Blood is drawn and placed in a centrifuge, separating platelets from other blood components.
- Injection: The concentrated PRP is injected into the knee joint under sterile conditions.
- Mechanism of Action: Platelets release growth factors that stimulate cellular repair, reduce inflammation, and improve joint function.
PRP’s role in managing knee arthritis lies in its ability to enhance the body’s natural healing mechanisms. Unlike temporary pain relievers, PRP focuses on the regenerative repair of cartilage and surrounding tissues.
Success Rates For Knee Arthritis
Studies and clinical trials have shown varying success rates for PRP in treating knee arthritis. While individual results differ, many patients report significant improvements in pain and mobility.
Evidence-Based Outcomes
Pain Reduction:
- Clinical research demonstrates that PRP injections can effectively reduce chronic knee pain associated with arthritis.
- Compared to traditional treatments like hyaluronic acid, PRP often delivers longer-lasting relief.
Functional Improvement:
- Patients experience enhanced knee function and mobility post-therapy, with effects lasting up to 12 months in many cases.
- Younger individuals or those in early arthritis stages report greater benefits.
Comparative Studies:
- A 2018 feasibility study concluded that PRP provided symptom relief comparable to steroids and hyaluronic acid injections while being safer for long-term use.
Factors Influencing Success
- Arthritis Stage: Early-stage arthritis responds better than advanced conditions.
- Frequency of Injections: Studies suggest that multiple sessions, spaced a few weeks apart, yield optimal outcomes.
- Patient Health: Non-obese patients and those with fewer comorbidities tend to achieve better results.
Despite promising results, PRP is not a universal cure. It should be viewed as part of a comprehensive treatment plan, including physical therapy and lifestyle modifications.
Leukocyte-Rich PRP vs Leukocyte-Poor PRP: When to Use Each
When it comes to PRP therapy, the type used can significantly affect the outcomes for knee arthritis patients. PRP exists in two main forms: Leukocyte-Rich PRP (LR-PRP) and Leukocyte-Poor PRP (LP-PRP). Understanding when to use each type is crucial for achieving the best results.
Leukocyte-Rich PRP (LR-PRP)
LR-PRP contains a higher concentration of white blood cells (leukocytes), which can increase inflammation. This type of PRP is typically used for tendon injuries or tendonopathies, where inflammation and tissue repair are key components of the healing process.
- Ideal for: Tendonopathies, where inflammation is part of the healing process.
- Not ideal for: Knee arthritis, where excessive inflammation could worsen the condition.
Leukocyte-Poor PRP (LP-PRP)
LP-PRP, on the other hand, contains fewer white blood cells, making it a better choice for knee arthritis. It focuses on tissue regeneration and inflammation reduction without triggering excessive inflammatory responses.
- Ideal for: Knee arthritis, where reducing inflammation and promoting cartilage regeneration is the goal.
- Why it works for knee arthritis: LP-PRP promotes healing without exacerbating inflammation, helping to slow the progression of arthritis.
Selecting High-Quality PRP: What to Look For
Not all PRP preparations are the same. To maximize the effectiveness of the treatment, it is essential to choose high-quality PRP with the following characteristics:
1. High Platelet Concentration
A higher concentration of platelets—typically 3-5 times higher than baseline—can increase the effectiveness of PRP. Platelets contain growth factors that stimulate healing, so a higher concentration means more potential for tissue repair and regeneration.
2. Adequate Volume
Depending on the joint or area being treated, sufficient volume is needed to ensure that the therapeutic effects are delivered effectively. This ensures that the PRP can adequately address the affected tissues in the knee joint.
3. Advanced Processing Technology
The method used to prepare PRP greatly influences its quality. Choose a system that can precisely control the platelet count and leukocyte content, ensuring the PRP is tailored to the patient’s condition. Not all systems are equal in terms of preserving platelet integrity and bioactivity, which is critical for clinical success.
What Patients Should Know

If you’re considering PRP for knee arthritis, understanding the procedure, risks, and expectations is crucial.
The Procedure
- Preparation: Patients should avoid anti-inflammatory medications (e.g., ibuprofen) a week before the procedure to maximize PRP efficacy.
- Session Duration: The entire process takes approximately 30-45 minutes, including blood draw, processing, and injection.
- Post-Injection Care: Patients are advised to rest the knee and avoid strenuous activities for at least 48 hours post-procedure.
Benefits of PRP
- Natural Treatment: PRP utilizes your own blood, eliminating the risk of allergic reactions or disease transmission.
- Minimally Invasive: No surgery or extended recovery periods are required.
- Targeted Relief: Growth factors directly address the damaged tissues.
Risks And Side Effects
While PRP is generally considered safe, patients should be aware of potential side effects:
- Temporary pain or stiffness at the injection site.
- Minimal risk of infection due to the invasive nature of the procedure.
Ideal Candidates
PRP may be suitable for:
- Individuals with mild to moderate knee arthritis.
- Patients seeking alternatives to surgery or who are not responding well to other treatments.
- Active individuals looking to regain mobility and reduce discomfort.
FAQ
How soon can I expect results after a PRP injection?
Results typically begin to appear within a few weeks, with significant improvements often seen after 3-4 sessions.
Can PRP therapy prevent knee replacement surgery?
While PRP cannot reverse severe joint damage, it may delay the need for knee replacement by improving joint function and reducing pain.
Is PRP therapy covered by insurance?
Most insurance plans do not currently cover PRP therapy as it is considered experimental or elective. Check with your provider for specific details.
What should I avoid doing after a PRP injection?
Avoid heavy lifting, high-impact activities, and anti-inflammatory medications for at least two weeks post-injection.
How does PRP compare to corticosteroid injections?
PRP offers longer-lasting relief and focuses on tissue regeneration, whereas corticosteroids provide short-term pain relief by reducing inflammation.
Conclusion
Platelet-Rich Plasma (PRP) therapy offers an innovative, minimally invasive option for managing knee arthritis. By leveraging the body’s natural healing abilities, PRP can reduce pain, improve joint function, and delay the progression of arthritis. However, it is essential to consult a qualified healthcare provider to determine if PRP is the right treatment for your condition.
As research continues to validate its efficacy, PRP for knee arthritis remains a beacon of hope for those seeking relief from this debilitating condition. With proper preparation, realistic expectations, and professional guidance, patients can make informed decisions to improve their quality of life.
Whether you’re considering your first PRP session or seeking alternatives to traditional arthritis treatments, remember that a proactive approach and understanding the procedure can pave the way to better outcomes.
References
Glynn LG, Mustafa A, Casey M, et al. Platelet-rich plasma (PRP) therapy for knee arthritis: a feasibility study in primary care. Pilot and Feasibility Studies. 2018;4(1):93. doi:10.1186/s40814-018-0288-2. Source
O’Connell B, Wragg NM, Wilson SL. The use of PRP injections in the management of knee osteoarthritis. Cell Tissue Res. 2019;376(2):143-152. doi:10.1007/s00441-019-02996-x. Source
Pourcho AM, Smith J, Wisniewski SJ, Sellon JL. Intraarticular platelet-rich plasma injection in the treatment of knee osteoarthritis: review and recommendations. Am J Phys Med Rehabil. 2014;93(11 Suppl):S108-S121. doi:10.1097/PHM.0000000000000115. Source