When you’re knee is in pain and mobility has been decreased, a knee replacement surgery may be the best solution. One of the most promising developments in knee replacement surgery is tourniquet-less knee replacement – a technique that allows for knee replacements with minimal use of a tourniquet. In this blog post, we will discuss what tourniquet-less knee replacement surgery is, how it differs from traditional knee surgeries and what you can expect for pain control.
A tourniquet-less knee replacement does not require compression cuffs to stop blood flow during surgery as traditional knee replacements do. These cuffs can cause pain and swelling in the knee after surgery. These surgeries also reduce the risks of complications caused by tourniquets – including nerve damage or an increased risk for infection.
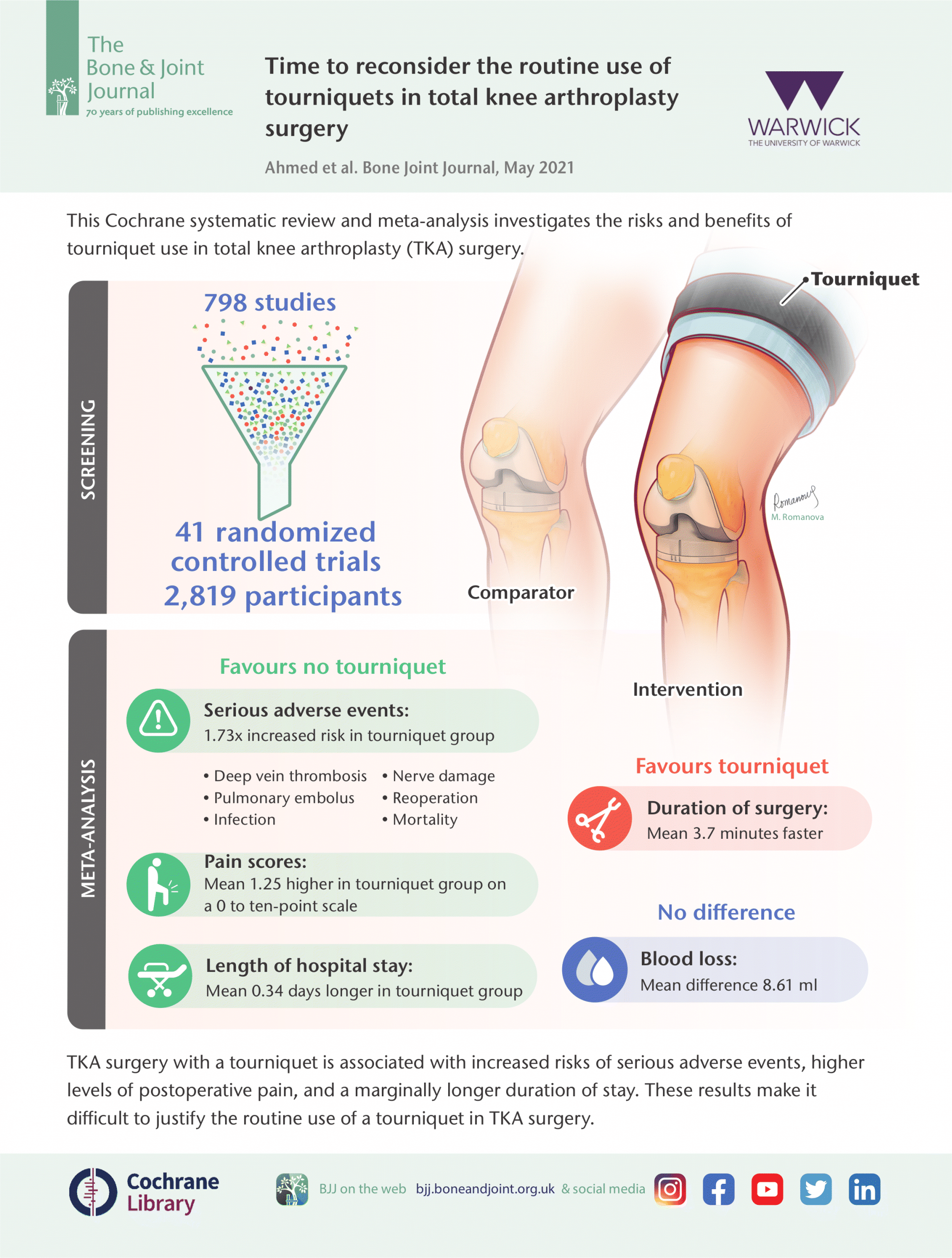
Tourniquet usage has been a standard component of total knee arthroplasty (TKA) since its inception. Tourniquet usage during TKA has attracted concerns in several research studies, although it is still a widespread practice.
The TKA procedure is a complex surgery with many steps that are required for a successful surgery and excellent long-term result. The improvement of that process may help patients save time and money while preventing harm.
Table of Contents
History of Tourniquet Use
The earliest tourniquets were made of cloth or leather straps wrapped around a piece of wood to tighten and were generally used in life-threatening emergencies and limb amputations.
The usage of tourniquets as a method for blood-loss control has been around since the days of Hippocrates. The pneumatic tourniquet, which was invented by Harvey Cushing, marked a significant step forward in this technology. Because these early pneumatic tourniquets sometimes had failures during power outages, they created a fresh set of problems. In the 1980s, microchip technology advanced sufficiently to allow for the creation of today’s tourniquet machines.
History of Tourniquets in Knee Replacement
In the United States, tourniquets are commonly used during knee replacement surgery. In 2010, the American Association of Hip and Knee Surgeons conducted a poll of its members, in which 100% said they used tourniquets at some point during knee replacement surgery. Another survey was conducted in 2019, and 88% of respondents still utilized a tourniquet during total knee replacement. In recent years, there have been several studies advising tourniquets to be abandoned in knee replacement surgery.
Tourniquet usage during TKA has several advantages. There is less blood loss when using a tourniquet. The use of a tourniquet provides a bloodless surgical field and better visibility. There’s evidence that there was less muscular damage and decreased inflammation. Tourniquets have been promoted as a way to reduce overall blood loss and improve cement fixation, but these claims have not been proved.
Cement Fixation
The need for revision may be caused by poor technique, so fixation is an essential component of a well cemented TKA. Improved fixation and implant survival have been observed with greater cement depth penetration. The more cement reaches into the bone, the easier it will interlock with the implant.
The risk of tourniquet-less TKA is that the depth of cement penetration may not be deep enough, and hence affect the implant’s longevity.
This belief was debunked by several studies. Researchers have found no difference in the depth of cement penetration, cement mantle thickness, or visible radiolucency between tourniquet and tourniquetless TKA operations.
The use of a tourniquet has not been shown to have an effect on implant migration or survival in short-term studies. In TKA without a tourniquet, it’s possible to penetrate the bone with cement and achieve secure implant placement.
Cementless total knee replacements do not have any concerns regarding the use of a tourniquet.
Blood Loss
There have been numerous studies conducted to examine blood loss and tourniquet use, and there has been a lot of blood loss without the use of a tourniquet.
The use of blood products during surgery is important as the need for transfusion carries significant health risks, including disease transmission, transfusion reaction, and infection.
The usage of tranexamic acid has largely reduced the incidence of allogeneic transfusion in knee replacement surgery. Several researchers have attempted to quantify the distinction between blood loss and transfusion rates depending on whether a tourniquet was used, and all of them revealed greater intraoperative blood loss in the no-tourniquet group but no difference in transfusion rates or overall blood loss has been definitively proven.
Postoperative Pain and Faster Recovery
The effect of tourniquets on recovery has been investigated in several studies. Tourniquet use may be accompanied by thigh discomfort and loss of quadriceps function.
In comparison to tourniquet use, TKA without a tourniquet has been shown to result in:
- less pain
- fewer analgesics used
- reduced leg edema
- improved range of motion and function after surgery
- higher success rates.
With the use of a tourniquet, TKA causes quadriceps function to be reduced for 3 to 6 months.
Tourniquet-induced neuropathy can be caused by direct compressive neurapraxia at the tourniquet site, and femoral nerve palsy has also been reported.
Risk of Complications with Tourniquet Use
The tourniquet causes an increased hypercoagulable state, stasis, and the potential for endothelial injury. This accounts for many of the reported complications involving the pulmonary and cardiovascular systems.
Tourniquet use can cause:
- compartment syndrome
- rhabdomyolysis
- cerebral infarction
- cardiac arrest resulting in death.
Conclusion
Tourniquet-less knee replacement surgery has many benefits and is becoming more popular. In fact, the Academy of Orthopedic Surgeons makes a strong recommendation that tourniquet-less total knees will lead to less postoperative pain and that this may lead to improved postoperative function. The use of a tourniquet may cause some complications, such as pain, higher blood loss during the procedure, or decreased quadriceps function. This doesn’t mean that it’s not possible to have a knee replacement with a tourniquet. Have a conversation with Dr. Morton about having a tourniquet-less knee replacement.
Sources:
- Stronach, Benjamin M. MS, MD; Jones, Richard E. MD; Meneghini, R. Michael MD Tourniquetless Total Knee Arthroplasty: History, Controversies, and Technique, Journal of the American Academy of Orthopaedic Surgeons: January 1, 2021 – Volume 29 – Issue 1 – p 17-23 doi: 10.5435/JAAOS-D-20-00321
- https://www.orthoguidelines.org/
- Infographic: Time to reconsider the routine use of tourniquets in total knee arthroplasty surgery