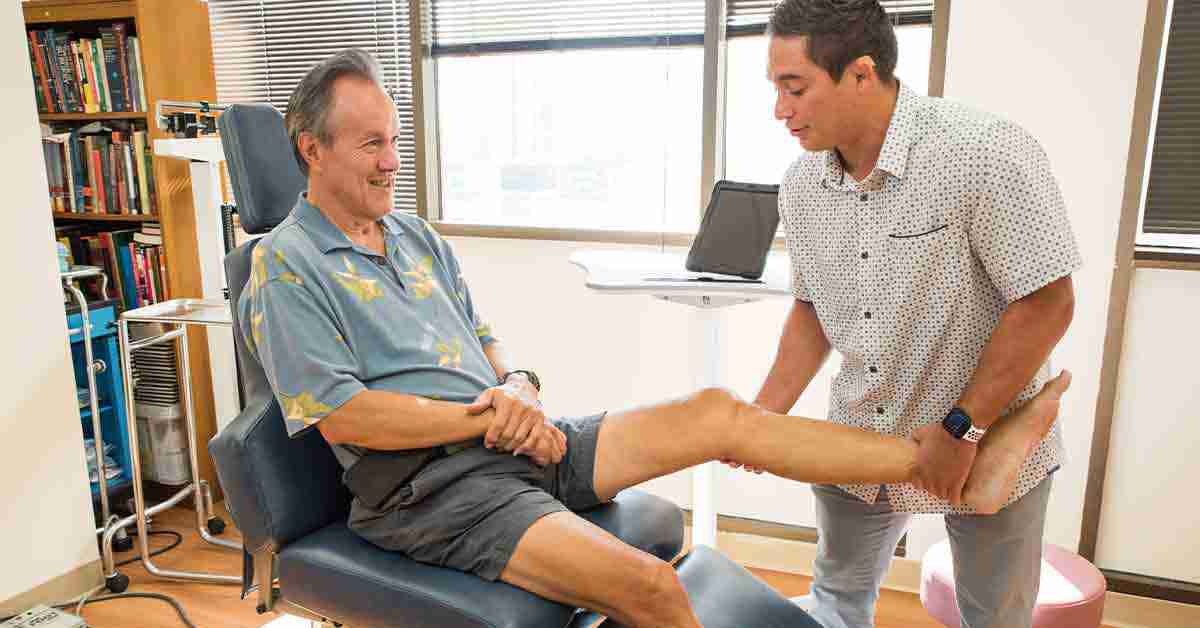
Pain is a critical part of our evolution. It works as a message from our brain to make us aware that something is wrong with our body requiring immediate attention.
The knee joint comprises three compartments: the medial compartment, the lateral compartment, and the patellofemoral compartment. The patellofemoral compartment consists of the space between your kneecap (patella) and thighbone (femur). The lateral compartment is the outside of the knee, while the medial compartment is the inside of your knee.
Inner knee pain is often an indicator of trauma or wear and tear to the cartilage, injury to the collateral ligaments, or other structures in the knee.
A clinical examination by the knee specialist with X-rays, ultrasound, and sometimes MRI (magnetic resonance imaging) is essential to determine the cause.
Common Causes of Pain on the Inside of the Knee
1. Osteoarthritis
Osteoarthritis affects millions of people. It results from wear and tears on your protective cartilage, which cushions the edges of your bones. Despite its ability to damage any joint, osteoarthritis most commonly affects the joints of your hips, knees, hands, and spine. Osteoarthritis symptoms are generally treatable, but damage to joints is hard to reverse. The best way to manage the disease is to stay active, maintain a healthy weight, and take some treatments.
Surgical procedures that involve replacing a joint are sometimes deemed the “last resort” treatment among people with osteoarthritis. Although many doctors recommend delaying joint replacement, you shouldn’t put it off for too long if you want the best results.

2. Anteromedial arthritis
The anterior medial compartment refers to the side of the knee closest to the front of your knee. Anteromedial arthritis is wear that occurs in the front part of the inner compartment of the knee.
Anteromedial arthritis results from the gradual wear away of the smooth cartilage at the ends of your bones. This causes the bones to rub against one another, causing medial knee pain. Patients with this type of arthritis usually have an intact ACL (anterior cruciate ligament), which prevents wear in the back of the knee.
Ultimately, the joint space can decrease, leading to the formation of bone spurs. It is common to feel inner knee pain in the evening or the following day after exercising. In some cases, there is swelling too. Diagnosis involves the use of X-rays or MRIs to assess the knee joints. This type of osteoarthritis is distinct on a clinicopathological and radiographic level and can be diagnosed with lateral radiographs. Unicompartmental arthroplasty (partial knee replacement) is the most appropriate treatment.
3. Rheumatoid arthritis
Rheumatoid arthritis (RA) is a disease that damages joints throughout the entire body. A joint injury caused by RA tends to occur both on the left and the right side.
In other words, if you have pain in one knee joint, you will likely have the same pain in the other knee joint. Treatments for RA work best when the condition is detected early.
Inflammation and joint pain are common symptoms of RA. Exacerbations and flares refer to periods of increased RA pain and other symptoms. During other times, the symptoms disappear entirely. This is called remission. Unlike osteoarthritis, rheumatoid arthritis usually does not require surgery. However, some people may choose joint replacement surgery to reduce their joint pain and improve their quality of life.
4. MCL tear
The MCL medial collateral ligament joins the thigh and lower leg. The MCL runs inside the knee, and the lateral collateral ligament (LCL) runs on the outside. They help to hold the knee in its place.
An MCL injury is common in contact sports. When the outside of the knee gets directly struck during a collision, the knee can get thrown sideways. This can cause the MCL to tear. During running and turning, the muscle can further tighten and strain or tear the ligament.
A torn MCL triggers inside knee pain. Spraining the MCL causes less pain than tearing it. At the time of the injury, the person may hear a popping sound. MCL treatment includes physical therapy and ice. In rare cases, surgery may be required.
5. Medial meniscus tear
The meniscus is the cushioning cartilage located between the shinbone and the thighbone. Meniscus tears cause inside knee pain, swelling, and stiffness. Your knee might also seem like its motion has been blocked, and you might have trouble fully extending it.
Meniscus tears are sometimes self-healing injuries. There are multiple types of meniscal tears – and some won’t heal until they are treated. Standard therapies include rest, ice, and medication. In some cases, patients often require surgical repair for the affected meniscus.

6. Pes anserine bursitis
This condition causes inflammation of the bursa located between the shinbone and the hamstring tendon inside the knee. As a result of inflammation and excessive fluid production, the bursa swells, placing pressure on adjacent knee areas.
Bursae are jelly-like pouches located around the shoulders, elbows, hips, knees, and heels in the body. Their fluid content helps reduce friction between bones and soft tissues. They are located between bones and soft tissues, containing a small amount of fluid.
In pes anserine bursitis of the knee, you may feel pain inside your knee and tenderness in the area 2 to 3 inches below the joint. Rest, ice, and anti-inflammatory medication are among the treatments for this condition. Many patients feel relief after a corticosteroid injection to the area.
7. Medial plica irritation
Plicas are tiny folds on the thin tissue lining the knee joint. The average person has four on each knee. They allow for the smooth bending and extension of your leg.
Knee pain that originates in the anterior part of the knee most commonly results from medial plica irritation. In addition to pain, patients may complain of catching, locking, and crepitating on anteromedial surfaces of their knees while they are performing activities.
The medial plica irritation often results from an injury or overuse of the knee. If one starts exercising more than they usually do, this can trigger medial plica irritation. Trauma to the knee, such as a car crash, can also cause it to swell.
8. Knee contusion
Knee injuries that damage muscle or tissue are called soft tissue contusions. The symptoms of a bone contusion on your knee can be severe. Still, they share many similarities with those of mild tissue contusions. Bone bruises occur when there is an injury to the soft tissue beneath the surface of the bone. Knee contusions are relatively common. Treatment, recovery, and symptoms depend on how severe the damage is. In most cases, knee contusions are treated with the RICE protocol. The acronym stands for Rest, Ice, Compress, and Elevate.
9. Fracture
A knee fracture occurs when there is a broken bone. Fractures at the surface of the tibia on the inside of the knee are a severe cause of medial knee pain. An injury such as a fall or an impact at high speed usually results in a knee fracture. As soon as the damage occurs, people recognize there is something wrong and have difficulty bearing weight.
There are many symptoms associated with kneecap fractures, including
- Pain and burning sensations.
- Bruising and swelling
- The affected leg is unable to bend or bear weight
- During movement, there is a feeling of scraping or grinding
If you believe you broke a bone involving your knee, you should seek urgent consultation at an emergency department.

10. AVN
Avascular necrosis is a painful knee condition caused by the decreased blood supply to a part of bone in the thighbone or shinbone. Common AVN treatments include rest and taking pain medications. If you have advanced AVN, the knee specialist may recommend surgery to minimize damage and improve knee function.
AVN is a multistage knee condition. The first symptoms manifest as pain in the inner part of the knee. At an advanced stage, it becomes difficult to walk or stand on the affected knee. Treatments may include core decompression for early stages of avascular necrosis to joint replacement for late disease.
Home Treatments
In the event of significant inflammation such as severe osteoarthritis of the knee (with pain and swelling), NSAIDs (non steroidal anti-inflammatory drugs) can be an effective solution. These are drugs that aim to decrease or eliminate the symptoms caused by inflammation.
NSAIDs have anti-inflammatory and analgesic properties which make them useful in the treatment of joint pain. For example, in the context of rheumatoid arthritis, they will treat pain and stiffness in the morning.
Some non-drug-based strategies can also be used, particularly the RICE protocol, better known in sports medicine. It consists of 4 stages: Rest the injured knee, apply ice, and compress with a bandage and elevate it to reduce inflammation.
Nonoperative Treatments
Should your knee pain worsen after several days, or if simple at-home remedies fail to relieve it, you should see a doctor.
Following are some nonoperative treatments for knee injuries that Dr. Morton can help you with
- Steroid Injection: An anti-inflammatory medication that can help improve your pain and decrease swelling.
- Gel injection: A gel-like hyaluronic acid is injected into your knee
- Physical therapy: Exercises, stretching, and ultrasound can relieve pain and create a supportive environment for your knee to bear weight.
- Assistive device: When performing sports or everyday activities, wearing a knee brace may help by providing additional support.

Surgery: Arthroscopy vs. Joint Replacement
An arthroscopic procedure preserves the natural structure of the knee joint. In contrast, a knee replacement procedure replaces it with an artificial one.
In addition, the size of the incisions in arthroscopic surgery and knee replacements is another crucial difference. Three small incisions are necessary for arthroscopic knee surgery, each about a centimeter in length (less than half an inch). Knee replacement surgery, on the other hand, is an open procedure.
When determining the indication for a joint replacement on the hip or knee, the patient plays a decisive role. From a medical point of view, there is no “must” for an operation. Because it is not the x-ray findings of osteoarthritis or the degree of cartilage wear that are decisive for the surgical decision, but the patient’s level of suffering. For the latest technology, ask about robotic knee replacement surgery.
The most critical factor in the treatment algorithm is the patient’s level of pain. If your pain cannot be easily treated with nonoperative treatments, it is time to consider surgical intervention.
For personalized and innovative knee pain treatment in Hawaii, call Dr. Morton at +18084396201.